
Last week two cabinet ministers in Malawi died of COVID-19. Yes, you read that right. Two ministers in Lazarus Chakwera’s government died of COVID-19 in a single day…
So far 396 Malawians that have been lost to the pandemic, out of 16,049 confirmed cases. The deaths include two other high ranking government officials.
All deaths to COVID-19 represent a sad premature loss of life. And given that sombre picture, it’s easy for Malawians to be fearful, panic, or lose hope. In any case, if government officials who are viewed to have access to the best medical care (some with access to pricey private medical care) in the country are ‘perishing to the virus‘, to quote a friend, what hope is there for the poor masses?
But going forward requires decisive action because inaction is not an option. If we’re to deliver the kinds of results necessary to stem the spread of the virus, then certain painful measures need to be put in place.
President Lazarus Chakwera, in his press conference last week declared a state of national disaster, and appealed to the international community, UN Agencies, NGOs and the private sector for more assistance and contributions to meet the challenge of the pandemic. Chakwera also called for an emergency meeting of the Presidential Taskforce on COVID-19 to explore additional measures to combat the pandemic. He also instructed several of his ministries (Health, Homeland Security, Education, Civic Education, Local Government, Justice and Information) to work together with the Vice President to review Malwi’s COVID-19 guidelines for curbing the spread of the virus, and recommend to the Taskforce any amendments to be made to those guidelines, and enforcement of those guidelines.

All well and good. However, depending on what Chakwera means by ‘additional measures‘, and depending on what additional amendments the ministries will recommend, I believe a full lockdown is the only way to resolutely stop the spread of this virus in Malawi.
The reason that’s the only sure-fire way is because if you look at countries that have successfully managed to control the spread of the virus, especially those with minimal fatalities, a full lockdown was one of the most important key measures taken.
NEW ZEALAND

The Australasian country of New Zealand has had a total of 2,267 COVID-19 cases and 25 deaths. 2,178 people in New Zealand have recovered from COVID-19 as of today. The success of New Zealand lies in early decisive action the country took, declaring a stringent lockdown as early as March 26, 2020 and taking an approach designed to “flatten the curve” of infections. The entire country (apart from essential workers & essential businesses) was required to self-quarantine at home, and after 5 weeks the lockdown was lifted. During this time, most workplaces, schools and public meetings were closed. Contact Tracing and Quarantine for visitors was put in place, introducing border restrictions to Non-citizens/ non-permanent residents, with all arrivals (regardless of where they came from or their symptomology) being made to go into managed isolation or quarantine facilities (mainly repurposed hotels) for 14 days. Those in quarantine where required to take Covid-19 tests on day 3 and day 12 of their time in quarantine.
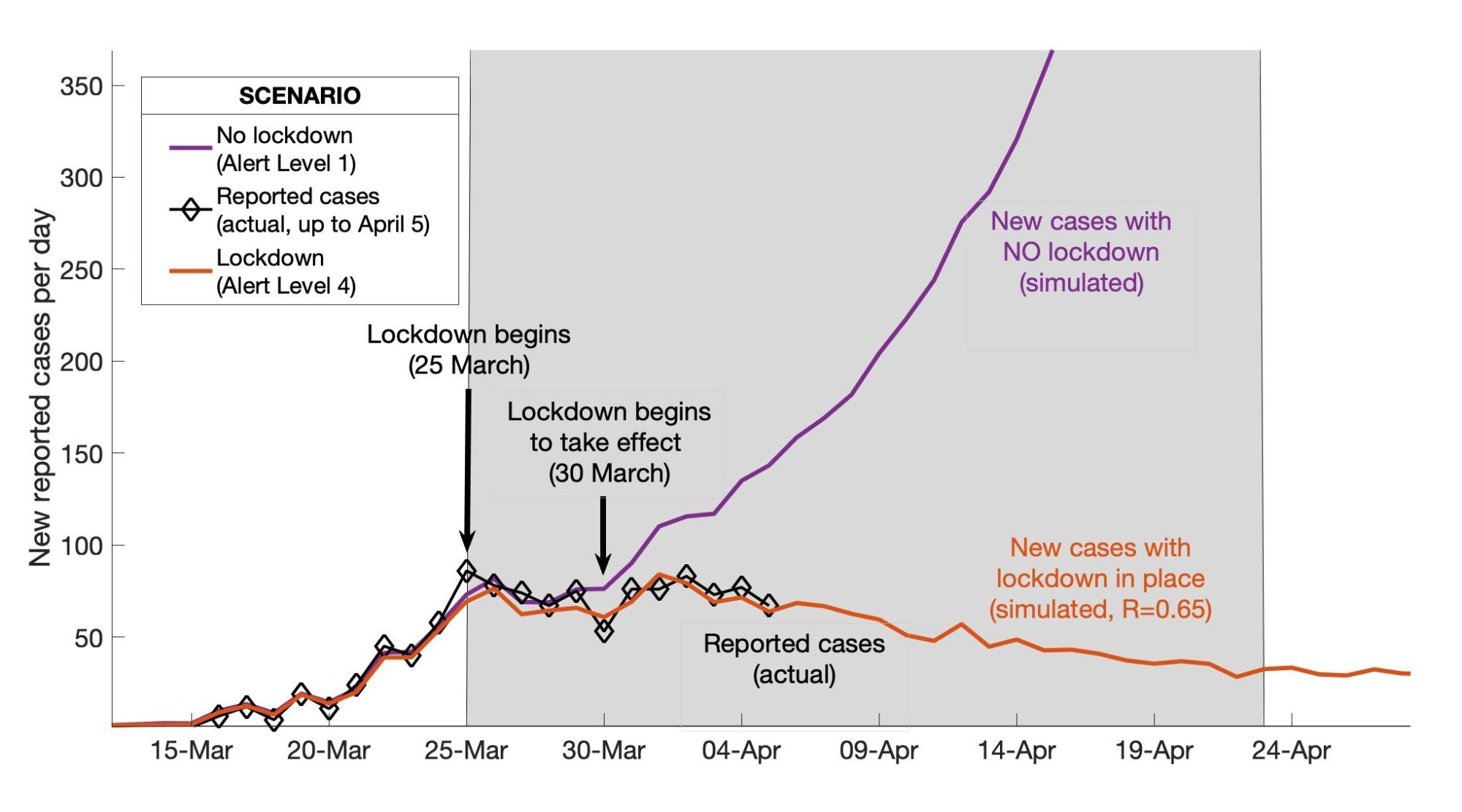
Public events were cancelled, and by May community transmission had been stopped, and in early June the Pandemic had been declared over in New Zealand. Following a further outbreak New Zealand brought in another lockdown in August 2020.
TAIWAN

Taiwan which has so far only recorded 7 deaths from COVID-19 from a total of 881 cases. After suffering from the SARS epidemic in 2003, the Taiwanese Centre for Disease Control very early in the pandemic begun screening all passengers arriving from Wuhan, and in collaboration with the Central Epidemic Command Centre (CECC – a body created to manage outbreaks, who in 2004 helped create a national health insurance smart card for each citizen, linking health records to travel history) ensured that each citizen had access to masks, and helped hospitals to be aware of potential COVID-19 cases in real time. The screening was soon extended to all arrivals from high-risk countries. Taiwan also created a digital quarantine system, whereby those who arrived from abroad were sent to a “quarantine hotel” – a hotel that has been repurposed for the pandemic – and were not allowed to leave their rooms for two weeks. This was supplemented by a track and trace system of in-person checks.
People who lived in a flat with their own bathroom were allowed to quarantine at home. Critically, those who were quarantining – be it in a hotel or at home – were monitored by a “digital fence” using their smartphones, cell towers and mobile phone carrier data. Anyone who ventured out of their area, was immediately contacted by text, and the health authorities informed – who would immediately send someone. If your phone run out of battery, a health officer would show up at your door.
The start of the new semester for schools was delayed for 2 weeks and by march there was a ban on large gatherings of 100 if indoors and 500 if outdoors.
In addition, citizens were paid monetary incentives, including £27 a day for staying in their room. Breaking the quarantines resulted in very high fines, as high as £27,000!
Taiwan also used the media to rebut false information, with press releases, viral memes and texts, encouraging wearing masks and importance of washing hands and using hand sanitizer. CoFacts, a collaborative fact checking service enabled those using chat apps to send something they suspected to be misinformation, to be fact checked.
LIBERIA

Liberia, which so far has recorded only 84 deaths from COVID-19, has had only 1,901 cases. Several lessons underscore Liberia’s Response to COVID-19
Strong Leadership — President George Weah took decisive action against COVID-19 in that after the first confirmed case on March 16, all travel was suspended if the countries of origin had more than 200 cases. In addition, Weah declared a national state of emergency as well as a 14 day stay-at-home order. Citizens were ordered to stay at home unless if going out shopping or to get supplies. Wearing masks in public was made mandatory.
Community Response — The Active Case Finders and Awareness (ACFA) Team, who had been instrumental in fighting Ebola, were instructed to fight against COVID-19 using many of the same tactics developed during Ebola, including recruiting and training contact tracers, setting up hand-washing stations as well as convincing businesses not to serve those not wearing masks.
Respect for Local Cultural Beliefs and Perspectives — To stem the spread of misinformation, the ACFA began to go door-to-door, while observing the social distancing guidance of 6 feet away from people, to follow contact traces as well as inform the community about facts of COVID-19, and to dispel myths.
Last Sunday, Chakwera said his government had released additional funding for use by various clusters of the Presidential Taskforce. He also outlined his priority in managing the recent surge of hospitalisation and providing emergency care to the critically sick, employing an additional 1,000 healthcare staff, among several measures.
But considering what the above countries have done, and contrasting that with the President’s measures, and looking at the rate of spread of the virus, I find that the measures announced on Sunday fall well short of what the country actually needs to stop the spread of the virus.
This is because the measures Chakwera has announced do little to stop community transmission, and do not prevent People coming into the country from abroad from breaking the self-isolation guidelines.
Also, since Pandemic fatigue has set in as wet weather makes going outdoor less inviting even in a country known for good climate, some people are still meeting friends (or people of different households) indoors, including in religious establishments like churches. This coupled with the open borders, in particular travel from South Africa and a large essential workforce, including people who have to go out every day for their sustenance (with many such people living in crowded or dense housing), has created a confluence of suitable conditions for the pandemic to flourish.
Prototyping & Product Development
And Malawi is not alone. Countries like Brazil, India and the UK have all experienced something similar as some people burdened by months of lockdowns and stringent restrictions have let their guard down.
Many of us relaxed our vigilance against the virus and now we are paying the price
Lazarus Chakwera, in a radio address on Sunday 10th January 2021
The rise in home remedies
The video above shows the many home remedies that have been suggested as preventative, alleviating or managing some of the effects of COVID-19. And while with the exception of only a few studies there doesn’t appear to be any consensus from health authorities across the world as to the efficacy of such remedies, there are indications from anecdotal evidence that some such remedies are effective.
I think health services in countries which do not have as many resources to procure medical equipment lose nothing prescribing some such sound home remedies, be they blue gum leaves or anything else, especially when there is some evidence as to their efficacy, and the remedy itself is undertaken while observing strict health and safety measures. To qualify this point, you may remember that even the World Health Organisation (WHO) has made mistakes, in that in January 2019, while some of us were advocating that everyone must begin wearing masks in all public places, the WHO said there was no evidence that masks are effective in stemming the spread of COVID-19?! Poor advice which even the British government fell for??! A few months later the WHO began recommending that everyone should wear masks…?!
Pioneering procedures
Similar to the issue of home remedies, I am of the persuasion that certain pioneering procedures for the treatment of COVID-19 need to be further investigated by our Medical Agencies in Malawi. And the above video shows one such example, trialed in this case by Dr Emmanuel Taban in South Africa.
Epidemiologists and Surgeons at College of Medicine in Malawi need to take note and begin seriously looking into this procedure, and the use of IVERMECTIN(see video above) and others that have been flagged, for example the testimony of Dr Pierre Kory below- which advocates using anti-inflammatory steroids in critical care.
Preventing Infection transmission
And while the numerous fundraising efforts are commendable and very much necessary considering the circumstances, preventing the spread of the virus means stopping the infection transmission from one person to another.
It means proactive measures beyond mere reactionary fire-fighting in epidemic response and virus containment efforts.
This includes stopping any and all gatherings of people anywhere in the country, from State House all the way to the Tavern. It means borders must be closed again as was the case last year, preventing visitors entering the country, and restricting domestic and international travel to only necessary travel by residents/returnees returning home, and goods vehicles bringing in medicines, fuel and supplies. It means everyone who comes into the country must be quarantined in state run isolation facilities for a period of at least 14 days. Such measures will create the conditions that make infection transmission difficult.
In any case, a busload of people from South Africa will probably carry a much higher risk of bringing and spreading further infections into the country, than goods vehicles drivers traveling alone or in pairs. Further, it’s probably easier to test, quarantine and trace a handful of drivers passing through border entry points every now and again, than quarantining busloads of passengers who are expected to self-isolate- even when the authorities know very well that such people would either go on to live with relatives (spreading the virus to them) or wouldn’t be able to stay indoors for 14 days, as they’d need to go out to buy food or to work.
This issue is important in light of recent figures which showed that migrants returning from South Africa accounted for 40% of Malawi’s COVID-19 cases.
Malawi is a deeply religious country and President Lazarus Chakwera appears to be doing his best. His conviction and Christian faith are treasured leadership qualities which Malawians should cherish in terms of not only bringing people together, inspiring hope in the ‘divine intervention’, but also in the pursuit of collective resilience when faced with a killer disease.
But beyond subservience to a divine power and coalescence of people’s resolve, Chakwera’s government will need actions that can be quickly implemented beyond words. The type of action that has delivered positive results elsewhere!
This is important because some Malawians are already voicing concerns regarding Chakwera’s lack of decisive action.
There are also allegations that the request for funds which the president put out doesn’t make sense when his “bloated” cabinet is costing the tax payers nearly K1.6 Billion.
But that aside, only the most effective measures will reassure Malawians that the Tonse Alliance government is up to the task. And in my view, those measures must include a full lockdown.
Vaccine

Malawi needs to procure thousands of emergency vaccine doses for healthcare workers. This is important so that those at the forefront and in frequent contact with the sick are protected from the virus. Appeals to Indian, Chinese, European & American Pharmaceutical companies should be made as a matter of urgency to procure vaccines first for healthcare workers, followed by doses for high risk groups.
But because getting a vaccine could take time, then a lockdown is one of the drastic actions which the government can take right now, to stem the spread, especially in light of the recent “South African strain” which some health experts are saying is easily spread, and which appears to be more deadly.
Who will pay for it?
I’m not suggesting that a lockdown is an easy step, but I strongly believe it is necessary to stop the spread of the virus. In any case, if you prevent the spread of the virus, people will not be getting sick, thus will not be needing to be hospitalised. Thus, in the absence of a vaccine, a lockdown is a measure that tackles the root cause, as opposed to tackling symptoms.
In terms of funding, some of the COVID19 funds that so far have been set aside by government or which Malawi is receiving from donors need to be diverted into community support, to help those who are most vulnerable with food and supplies. Here, US$50 million needs to be set aside for a huge logistical and food aid operation that involves teams of tested healthcare workers going around buying food locally and distributing such food to communities, so that these people can stay at home for 2 or 3 months. Such an operation should be repeated several times as more funds become available.
Further, if such healthcare teams could receive the vaccine before such an exercise, it would improve the efficacy of the exercise.
Otherwise, the K72 Million which Chakwera said had so far been spent on protections and social support cluster to sensitize the public on the increased risks and evils of gender-based violence during the pandemic as well as to support victims and their families with materials and cash transfer, is in my view not enough. A lot more needs to be done.
